|
10/31/2023 0 Comments Pathological complete response her2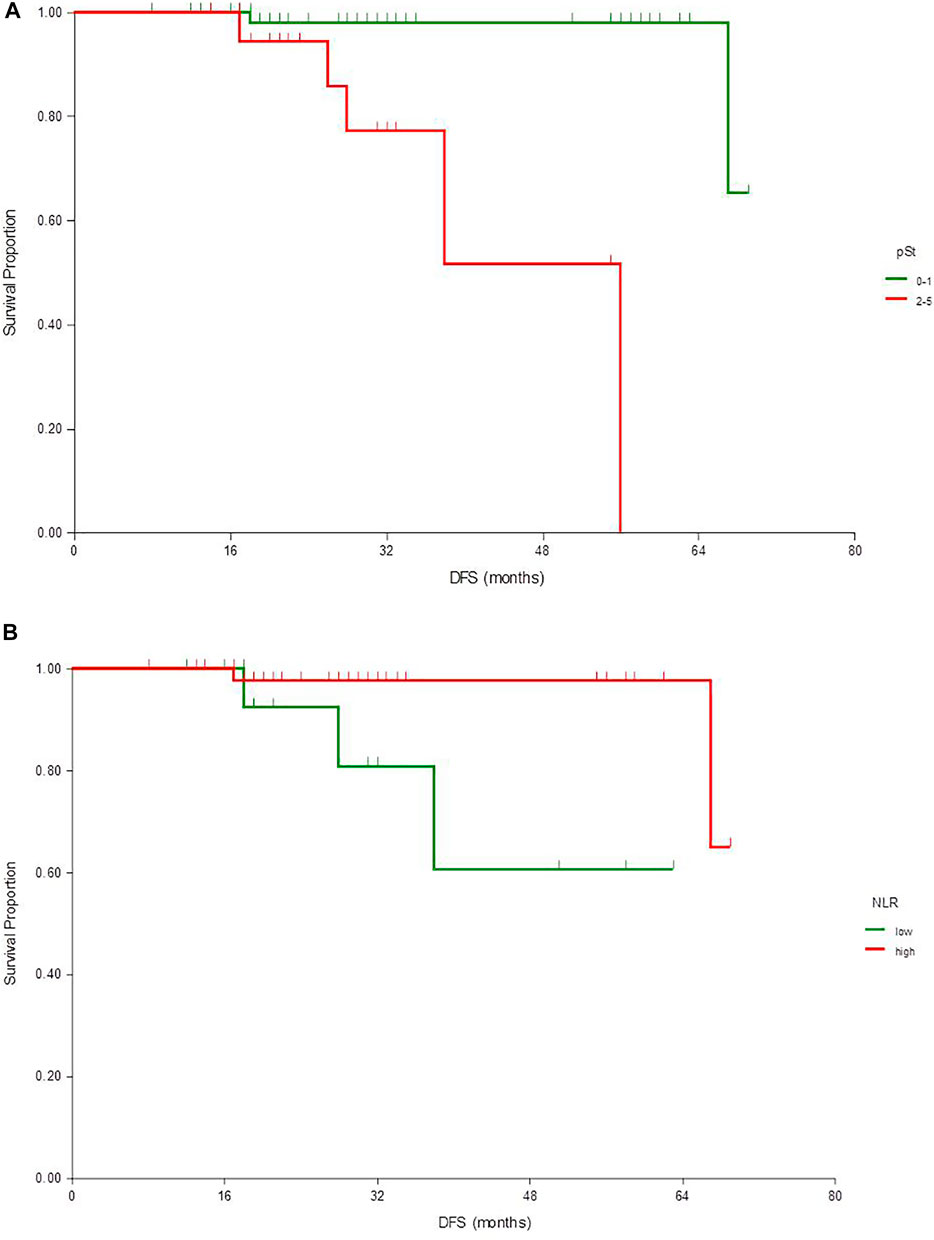
The aim of the present study is the retrospective evaluation of the predictive and prognostic role of HER2 expression levels in HER2+ BC patients receiving neoadjuvant treatment together with other clinico-pathologic variables as tumor infiltrating lymphocytes (TILs), histologic grade, residual tumor cellularity (RTC). The treatment with anti-HER2 drugs in BC patients is primarily based on HER2 protein overexpression established by immunohistochemistry (IHC) method, while “dual-probe in situ” hybridization (SISH) is used in case of HER2 with equivocal immunohistochemical score (IHC 2+). Identifying accurate and reliable biomarkers to predict response to HER2-targeted therapy in this subtype of BC has become a priority. 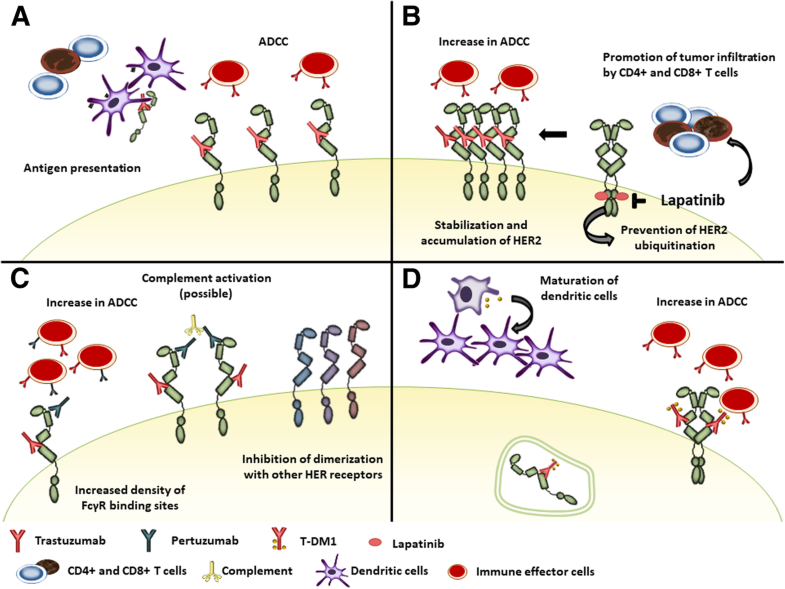
Several clinical trials proved that about 25–30% of HER2+ BC patients, treated with trastuzumab, after adjuvant chemotherapy experienced recurrence within 10 years of diagnosis 5, 10 and locoregional or distant recurrence has been identified after dual HER2-targeted neoadjuvant treatment (about 7.1% of cases) 11. Unfortunately, not all HER2+ BC patients have clinical improvement from anti-HER2 therapies. Chemotherapy, combined with dual anti-HER2 therapies, have been used as neoadjuvant treatment in HER2+ BC patients to improve the pathological complete response (pCR) rate 7 which is predictive for more favorable long-term outcome 8, 9. Currently, a combination of sequential chemotherapy and anti-HER2 drug is the landmark for patients with HER2+ BC subtype, both in the neoadjuvant, adjuvant and metastatic setting 6, 7. trastuzumab) have established a considerable upgrade in outcomes of patients affected by HER2+ BC subtype and modified the tumor natural biology 3, 4, 5. HER2 signaling triggers PI3K/AKT and RAS/RAF/MAPK pathways, boosting cell proliferation, growth, invasion, and angiogenesis in tumors 2. HER2 protein overexpression is observed in ~ 15–20% of all invasive breast cancer (BC), and it is associated to high invasiveness and worse prognosis if not properly treated 1. HER2 is a membrane glycoprotein with tyrosine kinase activity and a member of the epidermal growth factor receptor family. The combination of all predictors might offer new options for NACT effectiveness prediction and stratification of HER2+ BC during clinical decision-making. 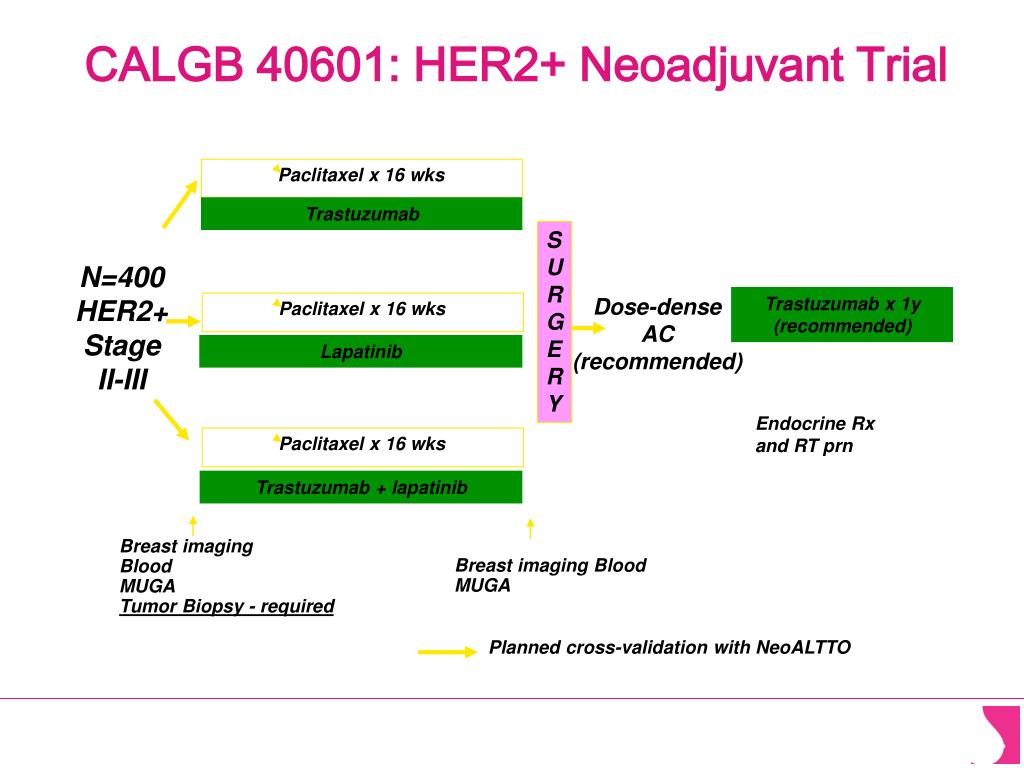
The immune microenvironment and scarce lymph node involvement have crucial role in clinical outcomes. Increasing TILs concentrations, lower lymph node ratio and lower residual tumor cellularity are associated with a better outcome. HER2 IHC3+ and G3 are poor prognostic factors for HER2+ BC patients, and could be considered in the application of neoadjuvant therapy. HER2 IHC score and laterality emerge as strong predictors of tumoral pCR after NACT from machine learning analysis. Better pCR rate correlate with a high percentage of infiltrating immune cells and right-sided tumors, that reduce distant metastasis and improve survival, but no incidence difference. 93.7% of ypT0 were HER2 IHC3+ BC, 6.3% were HER2 IHC 2+/SISH+ and 86.7% of ypN0 were HER2 IHC3+, the remaining were HER2 IHC2+/SISH+. High tumoral pCR show a scarce mortality rate vs subjects with a lower response. The tumoral pathological complete response (pCR) rate was 40.9%. We evaluate the predictive and prognostic role of HER2 protein/gene expression levels combined with clinico-pathologic features in 154 HER2+ BCs patients who received trastuzumab-based neoadjuvant chemotherapy (NACT). HER2+ breast cancer (BC) is an aggressive subtype genetically and biologically heterogeneous.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
